Pain on the Inside of the Ankle and Foot (Medial Side)
Tendonitis is a common foot problem as our feet take tremendous amounts of stress and rarely get to rest. The Posterior Tibial Tendon is particularly prone to problems as it must work constantly to support the arch of the foot.
If you think you may have posterior tibial tendonitis make an appointment right away to see us in our Seattle clinic. If not treated, this tendonitis can lead to a rupture or tear of the tendon.
Video: Inside of Foot Pain and Posterior Tibial Tendonitis Treatment
Home Treatment of Pain on the Inside of the Ankle and Foot (Posterior Tibial Tendonitis)
If you are not in the Seattle area and want to try home treatments first, you can find our recommended posterior tibial tendonitis self-treatments below .
Anatomy – Why is the Posterior Tibialis Tendon Prone to Injury?
The posterior tibial tendon starts deep in the calf and runs behind the ankle bone on the inside of the ankle. The tendon continues along towards the foot and attaches into multiple locations on the inside of the foot and the bottom of the arch.
A tremendous amount of tension and stress is placed is on this tendon with every step as it helps to maintain and recreate the arch of the foot. The amount of stress on the tendon varies from person to person depending on the shape of their foot (flatfeet versus a very high arch). It would seem that only a flatfooted person would get posterior tibial tendonitis is more common in flatfooted people, but it can occur in anyone.
Symptoms of Posterior Tibial Tendonitis – Pain on the Inside of the Foot
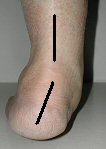
Figure 2 – Flattening of your foot causes outward rotation of heel promoting Posterior Tibial Tendonitis
Symptoms of posterior tibial tendonitis include pain and swelling along the inside of the ankle and arch along the course of the tendon.
There is often pain on the inside of the of foot.
Pain is present with walking, exercise or just standing. This discomfort will usually increase over time.
This pain initially is absent when at rest but may progress to the point where pain is present even when not active. In advanced cases the injury to the tendon that started as tendonitis may result in a full or partial tear of the tendon.
Diagnosing Posterior Tibial Tendonitis
We can usually make this diagnosis very easily by history and examination. Sometimes we will order an MRI or ultrasound to determine the extent of damage to the posterior tibial tendon.
Initial Treatment
Treatment can depend on how long the symptoms have been present and the amount of strength that is lost (if any) in the tendon. Initial treatment may include:
- First treatment is to decrease tension on the posterior tibialis tendon. This might include:
- Use of a walking boot
- Prefabricated or custom orthotics
- Taping or ankle braces
- Next, we need to reduce acute inflammation. This might include:
- Anti-inflammatory medication
- Icing
- Rest
- Physical therapy
- The next part of the treatment plan is to stimulate healing of the tendon. Depending on how you respond to the treatments above this may or may not be necessary. The most effective method to stimulate healing is shockwave therapy
Orthotics for Posterior Tibial Tendonitis
Orthotics for this problem are designed specifically to reduce tension on the posterior tibial tendon. This often requires an orthotic that is deeper than normal around the heel and perfectly matches the arch of the foot (total contact orthotics).
The correct orthotic can not only help heal the tendon by reducing tension on it but can also help prevent re-occurrence of the problem.
Depending on the level of treatment needed we may use a prefabricated orthotic with modifications to reduce tension on the posterior tibialis or a custom orthotic. Our goal is to use the least expensive therapy that will provide you with optimal pain relief.
Shockwave Therapy for Posterior Tibial Tendonitis
If we don’t see rapid improvement in your symptoms by reducing tension on the tendon and standard anti-inflammatory measures, then shockwave therapy is usually the next level of treatment.
Extracorporeal shockwave therapy is a safe and non-invasive therapy for many tendon disorders. The goal of shockwave therapy is to stimulate healing of tendon. It involves 4 – 5 sessions of shockwave therapy, each about 1 week apart. Treatments are usually not painful or cause only mild discomfort. Sessions take less than 15 minutes.
A number of studies have shown very positive outcomes using shockwave therapy for tendon disorders In a 2018 study of about 400 subjects, for example, “Shockwave therapy significantly reduced the pain that accompanies tendinopathies and improves functionality and quality of life. It might be first choice because of its effectiveness and safety”(1).
How Does Shockwave Work to Heal Tendon?
Shockwave therapy works by stimulating healing of tendon in two ways:
- New Blood Vessel Formation: Shockwave therapy helps create new blood vessels, a process called “neo-vascularisation”. The improved blood flow helps provide the nutrients that assist with tendon healing.
- Release of growth factors: Growth factors are proteins that stimulate the cells that repair tendon ()tenocytes).
How Effective is Shockwave Therapy for Posterior Tibial Tendonitis?
Shockwave therapy seems to work about 70% – 80% of the time to treat the pain of tendonitis. In a 2018 meta-analysis (analysis of multiple studies), “Extracorporeal shock wave therapy exerted a positive overall effect on pain and function for lower-limb tendinopathy. Shock wave types and dosage levels may have different contributions to treatment efficacy.”(2)
The British Medical Bulletin in 2015 noted in a systemic review that “Extracorporeal shock wave therapy (ESWT) is an effective and safe non-invasive treatment option for tendon and other pathologies of the musculoskeletal system.” (3)
As with all treatments, Shockwave Therapy has both advantages and disadvantages:
Advantages of Shockwave for Posterior Tibial Tendonitis:
- Acts to stimulate healing of the tendon which tends to provide long-term rather than short-term improvement
- Studies on most tendons show about 70 – 80% effectiveness at healing the tendon.
- An exceedingly safe treatment. There are no known risks or complications of shockwave therapy.
Disadvantages of Shockwave for Posterior Tibial Tendonitis:
- Shockwave does not provide rapid relief of pain. Because shockwave is working to essentially take tissue that has stopped healing and restart the healing process, improvement tends to be slow. Maximum clinical benefits are found at 12 – 20 weeks with an average of 16 weeks to maximum benefit.
- Shockwave therapy is not covered by insurance. The cost is $200 per session. Best outcomes are seen with approximatelly 6 sessions for a total of $1200. Ideally the first 3 sessions are done weekly. The final 3 sessions are done over the next 6 weeks.
- If we are treating two feet at the same time (or two locations on the same foot) the cost is $1900 for the 6 sessions.
- While there are many studies showing the benefits of shockwave for tendonopathies including the Achilles, gluteal, patellar and the rotator cuff, there are currently no high-level studies specifically on shockwave for the posterior tibialis. The physiologic effects should be the same, however.
How Many Sessions are Needed?
- Six sessions are recommended. Three initial sessions, each one week apart. Then the final 3 sessions over the next 6 weeks.
- We will see you back 16 weeks after the first shockwave session. At that time you should see maximum benefit from shockwave.
You can learn more about shockwave therapy here.
Treatment for Resistant Cases
This problem should be treated as early as possible in order to prevent damage to the tendon that can be more difficult to treat. Call us at our Seattle clinic right away if you are having symptoms.
In more severe cases a cast or walking boot from the knee down may be utilized from four to six weeks to allow the tendon to completely rest without placing the day-to-day demands of walking on it. An arch support or orthotic must be worn in the boot to support the arch and further reduce tension on the posterior tibial tendon. If these measures fail to produce acceptable results surgical intervention may be necessary to clean around the tendon and repair any defects in the tendon. Surgical repair is more commonly needed when there is a progressive weakness in the tendon. This loss of strength is called posterior tibial tendon dysfunction.
Taping for Posterior Tibial Tendonitis – Video
We often have our patients use special taping techniques to reduce tension on the posterior tibial tendon. We recommend the use of kinesiology tape since it does not irritate the skin as standard athletic tape often does. The video below shows proper technique for applying tape to protect the tendon.
Self Treatment Suggestions for Posterior Tibial Tendonitis and Pain on the Inside of the Ankle and Foot
Posterior tibial tendonitis and other causes of pain on the inside of the ankle and can sometimes be difficult to treat, so we do think you should see a podiatrist with a specialty in biomechanics. If you want to try home treatment first, use the following suggestions. If you are not better in 3 weeks, see a medical professional.
Keep in mind that treatment is focused on taking tension off of the posterior tibial tendon by supporting the arch of the foot. We recommend never going barefoot during this three week period of treatment. The following items are affiliate links and we will receive a small commission on items purchased.
Use an arch support in your shoes
An arch support, particularly one that conforms close to the arch of your foot, will act to support the arch and reduce tension on the posterior tibialis tendon. OTC arch supports will not work as w
For use in smaller shoes including high heels, flats, soccer cleats FootChair makes a much smaller orthotic that still has the adjustable height arch support. 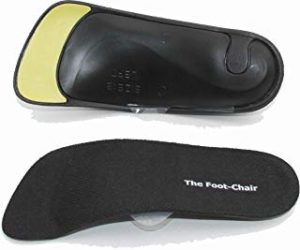

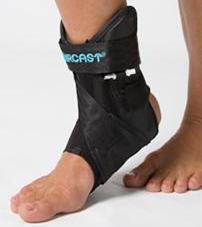
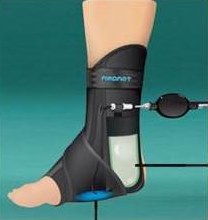

For more severe pain or longer lasting problems, wear a walking boot until you can see a medical professional. We recommend a high walking boot
Above all, don’t go barefoot at all for the first few weeks. Wear the ankle brace, walking boot, stable shoes with the orthotics or at least the sandals with arch support at all times when you are bearing weight. Usually the more support you have the fast you will heal, so the ankle brace or the boot should be worn for the first week or two and then transition into the shoes and arch supports.
Ice the inside of your ankle and foot two – three times per day for 10 minutes each time.
If you are not getting better or are not completely better within a few weeks, see a medical professional.
What are Other Causes of Pain on the Inside of the Foot and Ankle?
Although posterior tibial tendonitis is the most common cause of pain on the inside of the foot and ankle, there are other causes also. Those include:
- Stress fractures of the navicular or cuneiform bones
- Ligament sprains or tears in the midfoot
- Midfoot arthritis
- Tear of the posterior tibial tendon (a more severe form of damage to the tendon)
- Posterior Tibialis Tendon Dysfunction (a condition where the foot collapses due to a complete or partial tear of the posterior tibialis tendon)
The earlier you catch these problems the less likely you will have long term pain. If you are having any pain on the inside of your foot, make an appointment to see us in our Seattle clinic.
References:
(1) Effectiveness and Safety of Shockwave Therapy in Tendinopathies. Vasileios Dedes, et al. Mater Sociomed. 2018 Jun; 30(2): 131–146
(2) Efficacy of Extracorporeal Shock Wave Therapy for Lower-Limb Tendinopathy: A Meta-analysis of Randomized Controlled Trials. Liao CD, et. al. Am J Phys Med Rehabil. 2018 Sep
(3) Efficacy and safety of extracorporeal shock wave therapy for orthopedic conditions: a systematic review on studies listed in the PEDro database. Christoph Schmitz, et. al. British Medical Bulletin, Volume 116, Issue 1, December 2015




