Our Goal – Relief of Neuroma Pain without Surgery
Our goal is to relieve 100% of your Morton’s neuroma pain without surgery. We are extremely successful at providing relief in a conservative manner and we have a wide variety of treatments that we use to help cure your pain. Although neuroma surgery is usually effective, and we do perform it when necessary, every surgery has certain inherent risks so we always want to first treat conservatively. We will, however, recommend surgery in the rare event of having exhausted all non-surgical treatments.
Video: Treating Morton’s Neuroma Without Surgery
What Is a Neuroma?
If you have pain between the third and fourth toes of either foot, you may have a neuroma, also known as “Morton’s neuroma.”
This condition is usually caused by the bones on either side of the nerve pressing together to create pressure on the nerve. This can cause inflammation and fibrous thickening of the nerve leading to pain.
At the Foot and Ankle Center of Washington, we have developed a very effective and conservative treatment plan to treat neuromas so that we can relieve your pain without resorting to surgery. Contact us now for a consultation on pain-free feet.
What Are the Symptoms of a Neuroma?
Neuromas usually don’t have outward signs you can see on the exterior of your foot like a lump. Instead, you’ll experience discomfort between the third and fourth toe of either foot that can include shooting, burning, stabbing or radiating pain. It may feel like there is an object in your shoe, tingling, numbness or an odd feeling between your toes. Very often, the pain from neuroma will recede when you take off your shoes and massage the affected area.
What Causes Neuromas?
The exact cause is unclear, but those with high arches, flat feet or other biomechanical issues that cause instability around the toe joint are more susceptible to developing a neuroma. Foot trauma, tight or poorly fitting footwear that compresses the toes like high heels greater than two inches tall can lead to a neuroma. Slip on shoes are also a possible culprit. Repeated stress may also be a factor. Those that participate in sports or occupations that place undue stress on the forefoot may be more prone.
How Is a Neuroma Diagnosed?
In order to properly diagnose a neuroma and develop an effective treatment plan, clinical examination by a physician is required. The podiatrist will usually feel for a palpable click between the metatarsal heads. Diagnostic ultrasound imaging and x-rays of the foot to rule out other foot pathologies may also be recommended and will be determined on a case-by-case basis.
How Is a Neuroma Treated?
Doctors Hale and Huppin of the Foot and Ankle Center can usually relieve pain caused by neuromas without resorting to surgery and believe surgery should be used only as a last resort. We have great success treating neuromas conservatively, with less than 1% of our patients requiring surgery. In our experience, very few patients receive adequate non-surgical treatment options at other podiatric clinics.
Conservative treatment should include, at the very least, total contact orthotics designed to transfer pressure off of the ball of the foot and that are designed specifically to address neuromas.
Neuroma Treatment: Non-Surgical
Almost weekly, we see patients who have seen other podiatrists or orthopedists and who have only had steroid injections for treatment. When steroid injections failed to relieve their pain, they were told that surgery was their only alternative. In fact, while steroid injections are an important part of neuroma treatment, they are not likely to provide 100% relief as a stand alone treatment. If you have been told you need surgery for treatment of a Morton’s neuroma, make an appointment to see us right away for a second opinion. Surgery should only be a last resort.
There are a number of other treatments that should be tried before considering surgery including:
- Orthotics
- Shoe changes
- Corticosteroid injections
- Sclerosing injections
- Shockwave therapy
Orthotics to Treat Neuroma Pain
A recent study demonstrated that custom foot orthotics provided relief for Morton’s neuroma in 63% of patients. Reducing pressure on the ball of the foot is a critical aspect of treating a foot neuroma. Most of the orthotics made for this problem are ineffective because they gap away from the arch of the foot. In order to transfer pressure off of the ball of the foot and transfer it to the arch, the orthotic must conform almost airtight to the arch of the foot.
Video: Foot Orthotics for Morton’s Neuroma and Other Causes of Ball of Foot Pain
Read more here on how orthotics should be made to treat Morton’s neuroma – these are called Total Contact Orthotics. High heels (which can be very painful with a neuroma) and other dress shoes require very low profile orthotics, although it is still critical that the orthotics conform extremely close to the arch of the foot. Unfortunately, most orthotics are made are too large for those shoes.
In order to ensure the best outcomes from your orthotics, we first perform a detailed examination, including slow motion video analysis, of how you walk and your feet work. We then take a mold of your foot in a very specific position and the orthotic devices are prescribed in a manner to best reduce force and trauma to the area of your neuroma. If you already have orthotics, be sure to bring them with you to your appointment with one of our podiatrists.
Best Prefabricated Orthotics for Morton’s Neuroma
If you are not able to obtain a custom orthotic we suggest the FootChair Podiatrist Designed Orthotic with adjustable arch. This has the best arch height we have found on an over-the-counter arch support to transfer pressure off your forefoot as it is the only prefabricated orthotic with an adjustable arch.
The arch on the FootChair can be raised via pads that can be inserted under the cover. The higher the arch the less pressure there is on the neuroma. If you get a FootChair Orthotic we suggest using the maximum arch height that is comfortable for you.
For dress shoes (high heels and flats) and smaller sport shoes (such as soccer cleats) FootChair also makes a much slimmer profile 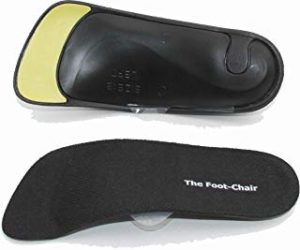 orthotic with the same exceptional adjustable arch support. The FootChair Slim Orthotic will fit in high heels. cleats and other low profile shoes. It also flexes to adjust to most heel heights.
orthotic with the same exceptional adjustable arch support. The FootChair Slim Orthotic will fit in high heels. cleats and other low profile shoes. It also flexes to adjust to most heel heights.
Shoe Changes for Foot Neuromas
Athletic and Walking Shoes for Neuromas
Athletic shoes should have a wide toebox to prevent compression of the neuroma.
Dress Shoes for Neuromas
Finding athletic shoes that work for people with neuromas is pretty straight forward but finding fashionable dress shoes for women that won’t hurt your neuroma is more of a challenge. You should look for the following features:
- Wide enough not to squeeze the toes
- A “rocker sole” to transfer pressure off of the ball of the foot and to limit tension on the nerves on the bottom of the foot.
- Accepts a dress orthotic or comes with an exceptional arch support.
We often recommend Earthies shoes which are fashionable shoes that have all of the features to help women with neuromas in their feet. If you come in for a consultation, we can offer other suggestions for fashionable high heels and dress shoes that are better for those with neuroma.
Corticosteroid injections for Neuromas
In many cases, reducing the force on the neuroma with proper orthotics and shoes will relieve all of a patient’s pain. When it doesn’t, steroid injections are an excellent supplementary treatment.
Steroid injections are meant to shrink the size of the neuroma in order to reduce pain. They are an effective treatment, but are too-often considered the only non-surgical treatment. In fact, recent studies show that the combination of orthotics and steroid injections works about 85% of the time to treat Morton’s neuroma.
In most cases of series of 3 injections offers the best outcome. The injections are performed 14 – 20 days apart. Up to 3 injections has been shown to be very safe with minimal chance of complications. Due to the risk of complications, however, it is not recommended to do more than 3 injections in the same spot over a 12 month period.
Prior to the injection we numb your skin with a cold spray to lesson any injection pain.
Coritcosteriod injections should be supplemented with appropriate orthotics and shoes.
Sclerosing Injections for Morton’s Neuroma
If orthotics and corticosteroid injections do not completely relieve your pain (these work in roughly 85% of patients), we may recommend sclerosing injections. Also known as “chemical neurolysis”, this process uses a chemical to cause destruction of the enlarged nerve which deadens the nerve pain in the feet. It is an older treatment that has recently been shown in several studies to be an effective method to treat neuromas in 61%-89% of patients (study results varied) with much less risk than surgery.
This is actually a series of seven injections, given 14 days apart, made of ethanol (alcohol) mixed with a local anesthetic. The nerve tissue absorbs the ethanol which, over repeated exposure, destroys the portion of the nerve causing your pain. Before the injection we numb your skin with a cold spray to lesson any injection pain.
Advantages of sclerosing injections include:
- Good success rate
- Few complications
- No down time
- Minimal pain (we are expert at administering less painful injections)
- May prevent the need for surgery
- Much less expensive than surgery
Disadvantages of sclerosing injections include:
- Requires multiple trips to our office (usually 5 – 7 for best long term results)
- Occasional pain for a day or two following injection
NOTE: As of April 2020 sclerosing injections are no longer available due to a price increase of dehydrated alcohol. The cost of a vial increased from $130 to over $1000, with a minimum purchase of 10 vials. Unfortunately, this makes the treatment cost-prohibitive. You can read more about this issue here.
Shockwave Therapy
There have been two studies indicating that shockwave therapy may be beneficial in treating Morton’s neuroma. Both studies showed overall good outcomes with about 70% improvement.
Shockwave has been shown to be a very effective method to treat tendon and ligament conditions. The studies supporting it for these issues are very strong.
Shockwave works by stimulating healing of tissue through the release of growth factors and the formation of new blood vessels.
It is a completely safe treatment with no complications, so it is certainly something you could consider prior to neuroma surgery. There is a caveat, however.
While the two studies that are available showed shockwave to be very effective in treating Morton’s neuroma, they are somewhat poorly designed studies. Both of the studies used questionable statistical methods, so we don’t have as much confidence in these studies as we do the many excellent studies supporting shockwave for tendon and ligament conditions.
Neuroma Surgery
Neuroma surgery should be a treatment of last resort. Every surgery comes with the risk of complications and can leave you with pain worse than what you had before. Surgery cannot be undone. We have patients come to us after unsuccessful neuroma surgery at another clinic and a review of their records clearly shows that non-surgical treatment would likely have resolved their issues.
FAQs About Neuroma Surgery
Q. When is neuroma surgery appropriate?
A. At the Foot and Ankle Center of Washington, we use the following criteria to determine if a neuroma operation is indicated:
- Your neuroma was confirmed by examination, diagnostic injections and/or imaging
- You have tried physician-prescribed custom orthotics designed to treat neuroma
- You have tried shoe therapy, including modifications such as accommodative padding
- You have tried injection therapy
- None of these non-surgical therapies successfully treated your neuroma
- Your neuroma interferes with daily activities
In our experience, less than 2% of our neuroma patients require surgical treatment of the neuroma and the majority can be treated by the alternate means discussed above.
Q. How does surgery treat a neuroma?
A. The goal of neuroma surgery is to relieve the pressure caused by the enlarged nerve. There are a couple of ways to accomplish this. To our knowledge, there are no thorough studies that compare the two surgical procedures. The most common surgery is removal of the nerve and we usually opt for this approach as it seems to offer less chance pain will return later. Here are the two methods explained:
- The method we recommend is neurectomy – the complete removal of the nerve. The advantage is that there is more predictable relief of pain. However, a disadvantage is that removing a portion of the nerve leaves a numb sensation on a small portion of the toe.
- The other standard methods is to release the ligament between the metatarsal bones to reduce pressure that the metatarsal heads place on the neuroma. The advantage of this procedure is that the nerve is left intact which eliminates the possibility of a new neuroma (a “stump neuroma”) forming where the nerve was removed. The disadvantage is that the neuroma may continue to cause pain.
Q. Are all neurectomy procedures the same?
A. The simple answer is no. Neuroma surgery can be performed either from the bottom or top of the foot. An incision on the bottom of the foot (plantar approach) is more direct but may cause discomfort because it leaves a scar on the bottom of your foot. An incision on the top of the foot (dorsal approach) is usually better for most patients because it avoids the scar on the bottom of the foot. The only time we recommend the plantar approach is for patients that have had return of a neuroma after a prior surgery.
Q. What happens during and after neuroma surgery?
A. Surgery is usually performed under local anesthesia using IV medication to make you sleepy. After surgery, you will have to keep your foot dry for two weeks. For best results and the least pain, we recommend being non-weightbearing (using crutches or a knee-walker) for one to two weeks after neuroma surgery. After that, we recommend a walking boot for two to four more weeks. We have found that patients experience less pain and swelling if they protect their foot in the initial weeks after surgery.
Most patients can move into a regular shoe after this, but may still have some discomfort until the area completely heals and tissues remodel. We find that patients often do better long- term if they wear total contact orthotics in shoes after recovery from neuroma surgery. The orthotics decrease pressure under the surgery site on the ball of the foot. This is particularly helpful during the first months after surgery while the foot is healing.
Q. What is the success rate of neuroma surgery?
A. Some neuromas may reoccur but this is rare. Most studies on patient satisfaction after neuroma surgery show approximately 90% reduction of pain and about 85% of patients rated their satisfaction with results as excellent or good.
- What complications may result from neuroma surgery?
Every surgery carries the risk of complications. Even if the surgery goes off without a hitch and the patient does everything perfectly right post-op, some will still develop complications. This can include pain, infection or slow healing. Other complications, more specific to neuroma surgery, include:
- Numbness – This is common and will usually occur on the sides of the toes adjacent to where the neuroma was removed. Most patients will not notice this in day-to-day activity. There may also be some numbness on the bottom of the foot near the site where the neuroma was located.
- Callus – In rare cases, patients can develop a callus under the ball of the foot after neuroma surgery. This is likely due to changes in the way you bear weight while recovering from surgery.
- Continued or return of neuroma pain – Patients who chose the decompression surgery may continue to have problems if the size of the neuroma causes ongoing irritation.
- Development of another neuroma – Patients who opted for neurectomy may develop a stump neuroma (a second neuroma that forms at the surgical site) that may be even more painful than the original problem. This can be difficult to treat and may require another surgery if it doesn’t respond to non-invasive therapy.
- Metatarsal pain – This can result from removal of fat in the surgical area during the procedure.
- Pain from an adjacent neuroma – If you have more than one neuroma and only had one treated surgically.
Q. Is cryosurgery a good treatment option for neuroma?
A. Cryosurgery uses extreme cold to destroy the nerve tissue. We have evaluated cryosurgery for neuromas and have decided not to offer this as a treatment option for neuromas at the Foot and Ankle Clinic of Washington. There is currently very little research that shows it to be an effective treatment for Morton’s neuroma but, if better evidence emerges in the future, we will consider it at that time.
Q. How should you choose a physician for your neuroma surgery?
A. Some foot surgeons are exceptionally skilled at neuroma surgery, some are mediocre, but most are somewhere in-between. To ensure the best possible outcome, you should choose an experienced and skilled neuroma surgeon like the professionals at the Foot and Ankle Center of Washington. Click here to see our bunion surgery page on bunion surgery and scroll down to Who Should Perform Your Surgery? for tips on identifying good surgeons and those to avoid.
Q. What Will Happen If I Don’t Have My Neuroma Treated?
A. It is difficult to predict the outcome of an untreated neuroma and how it will progress. Usually, if a neuroma is untreated, the following occurs:
- Growth of the neuroma
- Increased discomfort and/or pain
- Inability to wear certain shoes
- Inability to perform some job duties
- Need for surgical removal
If you have been told you need neuroma surgery, make an appointment to see Dr. Hale or Dr. Huppin as soon as possible for alternative, non-invasive neuroma treatment. Even if you’ve been told by another doctor that neuroma surgery is your only option, you should get a second opinion from us, as our treatments have been proven as an effective alternative to surgery for 98% of patients. Please be sure to bring any shoes and orthotics you wear regularly when you come for your consultation.
Contact the Foot and Ankle Center to schedule an appointment to address your neuroma pain as soon as possible.
Medial References for Morton’s Neuroma
SB Weinfeld, MS Myerson, “Interdigital Neuritis: Diagnosis and Treatment,” Journal of the American Academy of Orthopaedic Surgeons, 4(6) (Nov 1996): 328-335.
MJ Coughlin, RA Mann, Surgery of the Foot and Ankle, 7th edition Mosby-Year Book (1999).
FM Thompson, JT Deland, “Occurrence of two interdigital neuromas in one foot,” Foot & Ankle International, 14(1) (Jan 1993): 15-7.
KA Levitsky, BA Alman, DS Jevsevar, “Digital nerves of the foot: anatomic variations and implications regarding the pathogenesis of interdigital neuroma,” Foot & Ankle International, 14(4) (May 1993): 208-14.
JL Thomas, EL Blitch 4th, DM Chaney, et al, “Diagnosis and treatment of forefoot disorders. Section 3. Morton’s intermetatarsal neuroma,” Journal of Foot and Ankle Surgery, 4(2) (Mar-Apr 2009): 251-6.
J Mulder, “The Causative Mechanism in Morton’s Metatarsalgia,” The Bone & Joint Journal, 33 (1951): 94-95.
R Rout, H Tedd, R Lloyd, et al, “Morton’s neuroma: diagnostic accuracy, effect on treatment time and costs of direct referral to ultrasound by primary care physicians,” Quality in Primary Care, 17(4) (2009): 277-82.
JD Mozena, JT Clifford, “Efficacy of chemical neurolysis for the treatment of interdigital nerve compression of the foot: a retrospective study,” Journal of the American Podiatric Medical Association, 97(3) (May-June 2007): 203-6.
RJ Hughes, “Treatment of Morton’s neuroma with alcohol injection under sonographic guidance: follow-up of 101 cases,” American Journal of Roentgenology, 188(6) (June 2007): 1535-9.
GL Dockery, “The treatment of intermetatarsal neuromas with 4% alcohol sclerosing injections,” Foot and Ankle Surgery, 38(6) (Nov-Dec 1999): 403-8.
B Saygi, “Morton neuroma: comparative results of two conservative methods,” Foot & Ankle International, 26(7) (July 2005): 556-9.
L Trotter, “The Short-term Effectiveness of Full-Contact Custom-made Foot Orthoses and Prefabricated Shoe Inserts on Lower-Extremity Musculoskeletal Pain: A Randomized Clinical Trial,” Journal of the American Podiatric Medical Association, 5(98) (Sept 2008): 353-363.
D Makki, “Efficacy of corticosteroid injection versus size of plantar interdigital neuroma,” Foot & Ankle International, 33(9) (Sept 2012): 722-6.
RE Musson, “Ultrasound guided alcohol ablation of Morton’s neuroma,” Foot & Ankle International, 33(3) (Mar 2012): 196-201.
C Akermark, “A prospective 2-year follow-up study of plantar incisions in the treatment of primary intermetatarsal neuromas (Morton’s neuroma),” Journal of Foot and Ankle Surgery, 14(2) (Feb 2008): 67-73.
C Akermark, “Plantar versus dorsal incision in the treatment of primary intermetatarsal Morton’s neuroma,” Foot & Ankle International, 29(2) (Feb 2008): 136-41.





