Bunion Surgery Guide | Seattle Bunion Surgeon
If you’re considering bunion surgery, it can be very confusing what options to pursue. There is a tremendous amount of information available, and much of it is contradictory whether it comes from your doctor, friends, the internet or family. This guide cuts through the clutter to assist you in making an informed decision. Be sure also to read our page on Bunions and Big Toe Joint Pain to get a thorough understanding of your condition in addition to the information on surgery.
We specialize in bunion treatment and, in most cases, we can treat the bunion pain conservatively. In fact, we feel strongly that surgery should be a last resort. Many patients are told surgery is their only option but then they come to us, and we can provide effective pain relief non-surgically. However, if conservative treatments have failed and bunion pain limits your activity, surgery can be a very effective option. If surgery is necessary you must ensure you see a specialist in bunion surgery.
Video: Don’t Have Bunion Surgery Until You Watch This Video
Consider these important and frequently asked questions about bunion surgery, surgeons, possible complications, and outcomes. Click a question to get the answers and information you need.
- When should you have bunion surgery?
- What are the types of bunion surgery?
- Which is the best bunion surgery?
- Who should perform your bunion surgery?
- Which surgeons should you avoid?
- Is a Podiatric Surgeon or Orthopedic Surgeon better?
- What do podiatric foot and ankle surgeons treat?
- What should you do to prepare for bunion surgery?
- What should you expect on the day of your surgery?
- What should you expect during recovery from surgery?
When should you have bunion surgery?
At the Foot and Ankle Center of Washington, we use the following criteria as a guideline when determining if surgery is indicated.
- You have a bunion as determined by clinical exam and x-rays.
- You have exhausted all conservative care including:
Functional orthotics – prescribed and cast by your doctor and designed to relieve pressure within the big toe joint.
Shoe therapy – including proper shoes for your foot type and activities and possible modifications to your shoes.
Accommodative padding
Activity modifications
Medications – short term therapy may help to reduce inflammation
Icing
Injection therapy – rarely used but may help in treating an inflamed bursa
- Your bunion interferes with daily activities.
- You have pain inside the joint.
- You would like surgery sooner than later.
What are the types of bunion surgery?
There are a number of different bunion surgery methods. The best procedure for one person is not necessarily the best for another. Some procedures allow you to walk much sooner meaning you may not have to use crutches. Depending on your foot type, some procedures have a greater risk for return of the bunion deformity. Other procedures may require you to be on crutches for a few weeks – but may offer a better long-term result.
Bunion surgery can be classified into two major categories – a head procedure and a base procedure. More recently, some patients have sought bunion surgery that is more cosmetic in nature. Below, we’ll explain the difference in these three surgeries.
Head procedure – surgery for smaller bunions
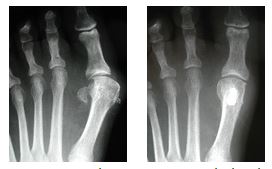
Head Procedure Bunionectomy – bone is cut just behind the joint and moved over. Fixated with screw (shiny area center of bone behind great toe joint).
Surgery for a smaller bunion is usually performed at the top of the metatarsal bone near the big toe joint. This is called a “head procedure.” To correct a smaller bunion, the bone is cut, and the head of the metatarsal moved over to correct the bunion. This procedure is usually indicated for a mild to moderate bunion or for patients who do not feel they can be non-weight bearing for any length of time.
Base procedure – surgery for larger bunions
Surgery for a large bunion is done near the bottom (or base) of the bone (closer to the ankle). This is called a “base procedure.” If you have a large bunion, doing the surgery at the head of the bone usually will not provide enough correction to give a good long term result. Base procedures are performed around the base of the 1st metatarsal. They include cutting a wedge out of the bone (base wedge), making a semi-circular cut and rotating the bone (crescentic osteotomy) and fusing the joint behind the great toe joint (Lapidus bunionectomy). Base procedures are usually indicated for a moderate to severe bunion.
Call 206-344-3808 or go here to schedule an appointment.
Cinderella Procedure® – cosmetic foot surgery
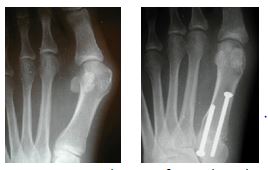
Lapidus bunionectomy – procedure performed at the base of the 1st metatarsal.
If you have bunions and have trouble fitting into shoes, you may have heard about the “Cinderella Procedure®” for bunions. The Cinderella Procedure® is a trademarked name for a type of bunion surgery that is designed to make the foot narrower in order to fit into smaller shoes.
It is very important to understand that the Cinderella Procedure® is not a new type of bunion surgery. It is simply a new name and a marketing campaign for a type of surgery that has been performed by podiatrists and orthopedic surgeons for decades. In fact, it is not a particularly sophisticated form of bunion surgery. It is a fairly simple procedure designed to “shave off” the enlarged bunion on the side of the foot in order to make the foot narrower.
Advantages and disadvantages of the Cinderella Procedure®
As with any bunion surgery, the Cinderella Procedure® has some advantages and disadvantages. The advantages are that it is a fairly simple surgery and, because the major bone of the big toe joint is not cut all the way through, you can bear weight on your foot fairly quickly. There are also have some very big disadvantages compared to other bunion surgery methods including:
- This procedure doesn’t work well for larger bunions.
- Procedures like this don’t correct the underlying cause of the bunion as well as other bunion procedures.
- Because the underlying problem is not corrected, there is a much greater chance of the bunion returning within a short time frame.
- You may have to have another bunion surgery after this one after your bunion returns.
We recommend that you fully pursue other non-invasive treatment methods before seeking surgery. And, if you do need surgery, we do not recommend the Cinderella Procedure® because it can lead to the need for another surgery later. We believe if you do have to have surgery, it should be a correct treatment that won’t require you to have a subsequent surgery.
Which is the best bunion surgery?
There is no one best type of bunion surgery. There are many variables in selecting a bunion procedure and the key to success is finding an experienced surgeon who understands each variable and who has the skill to perform all types of procedures. Some surgeons may not have the skills to perform base procedures, for example, and offer a head procedure as your only choice. You should avoid surgeons with limited capacity.
There is substantial medical research showing which bunion procedures are most effective in specific situations. At the Foot and Ankle Center of Washington, we perform an examination of your lower leg and foot and review biomechanics and x-rays. We then give you a complete explanation of your choices including what type of procedure is in your best interest. We do this in easy to understand terms and answer any questions you may have to ensure you clearly understand your options.
Who should perform your bunion surgery?
The most important criteria to ensure a good outcome for your bunion surgery is to choose the right surgeon. The qualities that make for a good bunion surgeon are:
- Board certified: You want a surgeon who is board-certified by the American Board of Podiatric Surgery (the only recognized surgical board) in Foot Surgery or Foot and Ankle Surgery. A more experienced surgeon will also be certified in Reconstructive Rearfoot/Ankle Surgery. (Note: Surgeons certified after 1990 are required to take and pass recertification examinations to ensure their skills are sharp. Those certified pre-1990 only self-assess.)
- Understanding of biomechanics: To choose the best procedure for you, a surgeon must also have the ability to evaluate your biomechanical structure including tightness of leg muscles, foot and leg alignment, motion of the bones around the bunion site, and midfoot and rearfoot alignment.
- Extensive experience: An experienced surgeon usually has the better ability to deal with complications that crop up during or after surgery and reduce the risk of these complications occurring. Numerous studies have demonstrated that one of the best predictors of surgical outcome is the experience of the surgeon.
- Gentle handling of tissue: A surgeon who handles tissue with a gentle touch will help ensure that pain is minimal and recovery time is reduced.
- Quality surgical facility: You want a surgeon who performs surgery in a peer-reviewed hospital or surgery center (not a surgery center located in the physician’s office).
- Honest communication: You want a surgeon who offers realistic expectations and explains the potential complications. Be wary of a physician who seems to talk you into surgery or makes surgery sound “too good to be true.”
- Use of post-op foot orthotics: Use of post-op foot orthotics: Bunion surgery does not usually alleviate all the forces that caused the bunion. The biomechanical cause of the bunion is often due to dysfunction in another part of the foot. Correcting the underlying biomechanical cause often involves very extensive surgery that is simply not necessary in most cases.
Instead, foot orthoses can improve biomechanical function and help prevent a return of the bunion. Orthotics can fit into many shoe types, including women’s dress shoes. If you already have orthotics, you will likely need new ones after surgery to match the new shape of your foot. Click here to find out more about custom orthotics.
Call 206-344-3808 or go here to schedule an appointment.
Which surgeons should you avoid?
Be very careful in your choice of surgeon. It is particularly important to avoid those that make unrealistic claims regarding surgical outcomes. If you see or hear the following statements from a potential surgeon, we suggest you pass on them and continue your search for a quality surgeon:
“90 plus percent of patients have pain free surgery”
Most surgeons could make that claim since surgery is usually performed with a local anesthetic, and the patient is sedated or asleep during surgery. After surgery, patients are usually given a long term anesthetic block to allow them to go home pain-free. Look for a surgeon who gives realistic expectations and does not make surgery sound too good to be true.
“I created a better bunion surgery”
There are several problems with this statement. First, all bunion surgery is a variation on several basic types of procedures. There have been substantial evolutions over the years, but if you hear anyone claiming that they have invented a procedure that is new and improved, you should have a healthy skepticism.
Second, there is no one best bunion surgery. The optimal procedure for you will depend on your foot shape, ligament tightness, biomechanics and other factors. Last, in most surgical specialties, if a truly better procedure is developed, it is adopted by most good surgeons.
“My patients never have a bunion return”
It is simply impossible to guarantee that a bunion will not return. The odds of a bunion returning are much less if the surgeon chooses the right procedure, and the patient follows all post-operative instructions. Also, the use of custom foot orthotics (specifically prescribed to enhance normal function of the big toe joint) after surgery can help prevent the return of bunions.
But the reality is that a very small percentage of bunions will eventually return regardless. Sometimes the forces leading to bunion formation are just too great. No surgeon can honestly guarantee they won’t ever return.
“My patients never require crutches”
This often means that the surgeon only knows how to perform a simple type of bunionectomy. More complex bunion procedures may require the use of crutches. In fact, even with a bunion procedure that allows early weight bearing, most surgeons will have their patients use crutches for a short period of time to reduce swelling and pressure on the surgical site.
“Surgery is performed in our own surgery center”
Be VERY cautious of a physician who performs bunion surgery in their office surgery center. To perform surgery in a hospital, physicians must pass a credentialing process, be approved by a committee to perform individual surgical procedures and re-credentialed/evaluated on a regular basis. This assures you the physician is fully qualified to perform your surgical procedure and does not have an impairment.
An office surgery center must usually be approved in order for them to bill Medicare, but the physicians are not regulated. A physician may be deemed not qualified to perform a procedure in the hospital, but this does not stop them from performing procedures in their own surgery center. A physician operating in their own surgery center has no one evaluating the quality of work. We tend to see more complications from patients who have had surgery in an office surgery center.
“I feel your bunion is going to get worse so you should have surgery as soon as possible”
Be cautious of a physician who does not suggest conservative therapies before suggesting surgery. There is currently no evidence in the medical literature that indicates that having bunion surgery earlier will prevent problems in later years.
“Surgery is virtually pain-free and minimally invasive”
Be wary of a physician who makes the surgery sound too good to be true. “Minimally invasive” bunion surgery was a term used many years ago to describe bunion surgeries performed through a very small incision. Due to significant complications with this type of bunion surgery, it is not currently recommended for bunion correction. A responsible surgeon will give you realistic expectations and review possible complications. Any surgery, bunion or otherwise, may have possible complications.
Is a Podiatric Surgeon or Orthopedic Surgeon better?
Both podiatric and orthopedic surgeons perform foot surgery. The question often arises as to which is more qualified. The reality is that it depends on the individual surgeon. There are exceptional podiatric foot surgeons and exceptional orthopedic foot surgeons. Conversely, there are mediocre surgeons in both professions.
From day one of their training, podiatric surgeons know they will be treating foot and ankle conditions, and receive in-depth education on these conditions as well as a broad education in general medicine. The first years of medical education for MDs, DOs, and DPMs are much the same. In fact, in many cases, the students are taught by the same teachers and in the same classes.
This general training in medicine allows both orthopedists and podiatrists to detect medical conditions affecting the lower extremities and deal with surgical patients who have medical conditions. Unlike other specialties, podiatric surgeons receive significant training in biomechanics during their education allowing a unique view of how foot surgeries can affect the lower extremity.
Board certified Podiatric Foot and Ankle surgeons are the surgical specialists of the Podiatric profession. American College of Foot and Ankle Surgeons (ACFAS) members are graduates of accredited US Podiatric medical schools, who have completed surgical residency programs of up to three years.
Fellows of the College are certified by the American Board of Podiatric Surgery, the surgical board for foot and ankle surgery recognized by the Joint Committee on the Recognition of Specialty Boards. Many have additional fellowship training in various aspects of foot and ankle surgery. All ACFAS members are dedicated to surgical excellence in the treatment of foot and ankle disorders.
Call 206-344-3808 or go here to schedule an appointment.
What do podiatric foot and ankle surgeons treat?
Foot and ankle surgeons treat a wide variety of foot and ankle conditions including:
- Structural conditions
- Trauma-related injuries
- Skin and nail conditions
- Congenital deformities
Foot and ankle surgeons are uniquely qualified to detect the early stages of diseases that exhibit warning signs in the lower extremities. They also manage those foot conditions that can pose an ongoing threat to a patient’s overall health. Such illnesses include diabetes, arthritis, and cardiovascular disease. In general an orthopedist who specializes in foot and ankle surgery completes a general residency in orthopedics and a one-year fellowship in foot and ankle surgery.
What should you do to prepare for bunion surgery?
- Arrange for a ride home after surgery.
- Do not plan on any long trips for at least two weeks after surgery.
- If you have significant medical problems, you may need medical clearance through your Primary Care Physician (PCP) since they know the most about your medical history. Schedule a physical with your PCP no more than 30 days prior to surgery.
- If you live alone, it is best to arrange for someone to stay with you for the first 24 hours after surgery.
- Wash your foot the night before and morning of surgery to reduce bacteria.
- Stop using anti-inflammatory medications five to seven days before surgery (this includes aspirin, ibuprofen, Advil, and Aleve).
- If you are taking any blood thinners, such as Coumadin, we will need to determine whether you can just stop the medication or go on a shorter acting blood thinner prior to surgery.
- Do not eat or drink anything after midnight the night before surgery.
What should you expect on the day of your surgery?
Surgery is performed in the hospital or a specialty surgery center. After most foot and ankle surgeries, you will go home the same day. You will generally be given a local anesthetic and anesthesia, and will be constantly monitored by an anesthesiologist. You will speak with the anesthesiologist prior to your procedure, and they will help you choose the best anesthesia based on your medical health and complexity of your case. Anesthesia choices are typically local anesthetic with sedation, general anesthesia, and spinal anesthetic. Most forefoot cases can be performed with local anesthesia and sedation.
After surgery, you will possibly be given a long-acting anesthetic to allow you to get home with minimal discomfort. You will also receive pain medication. You will need to arrange for a ride home as patients are not allowed to drive home on the day of surgery.
What should you expect during recovery from surgery?
Ability to bear weight on your foot after surgery depends on your procedure. A head procedure allows for immediate weight bearing, but we still feel that it is best to use crutches for one to two weeks. Base procedures require crutches for a longer period. Best results are achieved when patients are compliant with after surgery instructions. Here are some guidelines to follow after surgery:
- The first week after surgery, keep your foot elevated as much as possible.
- Keep your foot dry for at least two weeks after surgery.
- One week after surgery, you will have your dressing changed.
- The second week after surgery, your sutures will be removed.
- Your surgeon will advise you when you can increase weight bearing and activities depending on your procedure.
Meet our bunion surgeon: Dr. Douglas Hale
Bunion surgery should be the last choice of bunion treatment. We can usually eliminate your pain without performing surgery. But when bunion surgery is the last resort, we recommend Dr. Douglas Hale – our bunion surgeon and a renowned expert in bunion surgery. He is one of the few surgeons in the Northwest who is board certified in both Foot Surgery and Reconstructive Rearfoot/Ankle Surgery.
Dr. Hale is a graduate of the notable Northwest Podiatric Surgical Residency based at Swedish Medical Center, considered one of the five best Foot and Ankle Surgery Residencies in the country. He is the Director of the Foot and Ankle Surgery Residency at Swedish Medical Center. With more than 20 years experience performing many types of bunion surgery, Dr. Hale will recommend the bunion procedure that best fits your needs.
Hale’s philosophy is always to do what’s best for his patients. He feels it is so important to keep up on the latest procedures that he regularly participates in Grand Rounds at Swedish Medical Center (visiting patients with difficult medical and/or surgical conditions to evaluate and determine a treatment plan).
Click here to learn more about Dr. Hale, and if you have any questions after surgery with Dr. Hale, you are free to call him day or night to ask any questions about your post-op recovery or concerns.
Dr. Larry Huppin is a specialist in orthotic therapy and biomechanics here at the Foot and Ankle Center. If you want to avoid bunion surgery with orthotics designed to prevent bunions, make an appointment to see Dr. Huppin or Dr. Hale. Click here to learn more about Dr. Huppin.
Contact the Foot and Ankle Center of Washington to make an appointment with Dr. Douglas Hale to discuss your bunion surgery or to discuss options to avoid surgery. If this is for a second opinion, be sure to bring any x-rays or other tests you have available.




