What is a Plantar Fascia Rupture or Tear?
A rupture of the plantar fascia is a rip or tear in the thick plantar fascia ligament on the bottom of the foot. The tear can be complete (complete rupture) or just a portion of the fascia may tear (partial rupture).
What Does a Plantar Fascia Tear Feel Like?
Plantar fascia ruptures are very painful. Many people say that they felt a “pop in my arch” or a “pop in my heel” and then could not place any weight on the foot due to the pain.
What is the Treatment of a Rupture of the Plantar Fascia?
If you suspect a plantar fascia rupture, see a podiatrist immediately. Do not try to treat this yourself. If you are in the Seattle area, contact us for an appointment.
Current treatment recommendations for a complete tear are for patients to be treated for 2 to 3 weeks non-weightbearing using a removable cast boot.
If the tear is not complete we are often able to allow the patient to bear weight in a walking boot as long as the plantar fascia is supported adequately in the boot with a combination of an arch support that is modified to maximally reduce tension on the plantar fascia. In addition we will have our patients strap their foot. The entire goal is to reduce tension on the plantar fascia.
We will usually see you back after 2 weeks for evaluation and if you have been non-weightbearing have you start bearing weight in the cast boot.
In a 2004 study of athletes suffering from a tear of the plantar fascia, all 18 patients studied returned to activity (which included running, tennis, volleyball and basketball) within 26 weeks, with an average of about 9 weeks.
About the time you start bearing weight, we will talk to you about the use of custom or prefabricated orthotics designed to relieve tension on the plantar fascia. These will help get you back to activity sooner and also help prevent future ruptures.These are the same type of orthotics we use for plantar fasciitis.
Self Treatment of Plantar Fascia Rupture
This injury should not be self treated. We recommend you see a podiatrist or orthopedist.
If you absolutely cannot see a doctor right away, however, do the following until you can be evaluated. If for some reason you can’t see a doctor at all then you could so the following for about 3 weeks. We do recommend strongly that this condition should be evaluated by a doctor familiar with the foot and ankle injuries.
These are the products we recommend to our patients and they are also affiliate links so we may receive a small commission at no additional cost to you if your order from the link.
Wear a Walking Boot
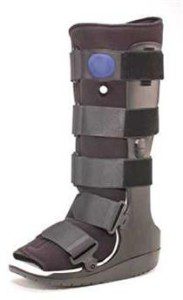
Wear a walking boot whenever you are weight-bearing. This should be a tall walking boot with a rigid rocker sole to reduce tension on the plantar fascia. We often recommend the United Fracture Boot as it is a quality boot at a fair price.
Use a Very Supportive Arch Support
Use an arch support in the boot. The support should be fairly rigid and conform as close as possible to 
We recommend the FootChair Podiatrist Designed Orthotic for it’s superior arch height and supportive construction. In addition it comes with arch pads that can be added to further increase arch height. This increased arch will more effectively reduce tension on the plantar fascia.
For smaller shoes including high heels, flats and soccer cleats, the recommended OTC arch support is the FootChair Slim Orthotic with 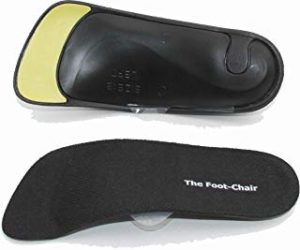
Wear a Plantar Fascia Sleeve
A plantar fascia compression sleeve will further reduce tension on the plantar fascia while reducing swelling and pain. Remember, the goal is to maximally reduce tension on the plantar fascia and the combination of the boot, the arch support will work to take maximum tension off of the plantar fascia.
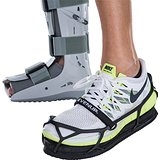
Use a Shoe Balancer to Keep Your Body Even When Wearing a Boot
Wearing a walking boot can make you uneven and lead to knee, hip and back pain. Using an Even-up Shoe Balancer on shoe of the other foot will keep you as even as possible and help to eliminate problems associated with wearing a fracture boot.
Treatment Plan Summary:
In the 2004 study, all patients returned to activity after 4 – 26 weeks. 14 of 18 patients returned to activity using custom orthotics to protect the plantar fascia. Mean time to return to activity was 9 weeks.
Week 1 – 3: Non-weightbearing or weightbearing with arch support and strapping
Week 3: Casted for custom orthotics
Week 3 – 6: Weightbearing in boot
Week 6: Begin weightbearing in shoe with custom orthotic. This orthotic should be a “total contact orthotic” in order to best relieve tension on the plantar fascia.
Causes of Plantar Fascial Rupture
Usually a rupture occurs after some sort of direct trauma to the heel, such as jumping from a height or a sharp blow to the heel or arch. Plantar fascia ruptures, however, do not usually occur all by themselves. There is usually a secondary condition that puts someone at risk for the rupture.
Plantar fascia ruptures are more likely to occur in people who have had long-term inflammation in the bottom of their foot (plantar fasciitis). This inflammation weakens the ligament and makes it more prone to rupture. A number of patients who develop a tear in the plantar fascia have had a history of steroid injections for treatment of plantar fasciitis, but it is unclear whether the ruptures are actually due to the steroid or to weakening of the plantar fascia due to plantar fasciitis.
Complications
Most patients do very well long term, but you have to be patient. You may not return to your previous activity for up to 7 months. We find that many patients become frustrated and feel that they are not improving because it can take so long to improve. But almost everyone has complete recovery if you give it adequate time. Very rarely, a lump may occur in the plantar fascia at the site of the rupture. This can usually be treated with orthotics, but in extremely rare situations is dealt with surgically.
References:
- Plantar fascia ruptures in athletes. Saxena A, Fullem B. Am J Sports Med. 2004 Apr-May;32(3):662-5.
- Incidence of plantar fascia ruptures following corticosteroid injection. Kim C, Cashdollar MR. Foot Ankle Spec. 2010 Dec;3(6):335-337
- Ultrasound evaluation of a spontaneous plantar fascia rupture. Louwers MJ, Sabb B, Pangilinan PH. Am J Phys Med Rehabil. 2010 Nov;89(11):941-4.